Yes. Your metabolism changes when you lose weight. Some of these changes are good, e.g. decreased fasting blood sugar, improved cholesterol measures, decreased storage of fat in places you don’t want it like your liver and waist, etc. Not all of the metabolic changes are good however, and in recent times there has been much discussion and handwringing over the role of metabolic adaptation (sometimes referred to as “metabolic damage”) in the setting of weight loss.
The idea is, given that body mass is controlled by the balance of energy expenditure versus energy intake, that in periods of caloric restriction, total energy EXPENDITURE is reduced — a feedback mechanism which serves to resist weight loss. In short, as you lose weight you burn less calories as a way for the body to protect itself from losing weight and this effect has been estimated to result in a decrease in daily energy expenditure of 30 calories per kilogram of weight lost. So, if you went from 100kg to 90kg then we’d predict that you’re going to expend 300 calories less per day than if you had not lost the 10kg or if you were originally 90kg and were maintaining your weight.
We have discussed elsewhere how the majority of this is mediated by a reduction in Non-Exercise Activity Thermogenesis (NEAT) – in other words, you spontaneously start moving around less, thanks to your brain trying to protect you from wasting away. This response should not be confused with metabolic damage or starvation mode, which at the time of this writing exist only on social media and not in the scientific literature.
Interestingly, there has been less emphasis on the effect of feedback mechanisms on total energy INTAKE during or after weight loss, partially due to difficulties in designing rigorous studies where energy expenditure is changed in a placebo-controlled manner in order to observe subsequent effects on energy intake.
In a 2016 paper by Polidori et al, researchers developed and validated a mathematical model for calculating energy intake changes over a 2-year-long period of time in a cohort of diabetic patients. They then employed a relatively new diabetes medicine known as Canagliflozin. This medication works by blocking certain channels in the kidneys that re-absorb glucose and prevent it from being “accidentally” excreted in the urine. By blocking these channels, the kidneys no longer re-absorb sugar as efficiently, and it ultimately gets peed out, resulting in improved blood sugar control in diabetic patients, as well as a bit of weight loss. Treatment with 300 mg per day of Canagliflozin results in an constant average excretion of 90 grams of glucose per day. This provides a novel way to manipulate energy balance without the awareness of study subjects, and can be used in a placebo-controlled fashion.
The researchers compared 153 subjects receiving Canagliflozin to 89 patients receiving placebo. Over the 52-week study, mean bodyweight declined in the Canagliflozin group (as expected, given the constant excretion of sugar), but subsequently stabilized at a new equilibrium point about 3.5 kg lower. In contrast, the mean bodyweight loss in the placebo group was less than 1 kg. (Fig. 1)
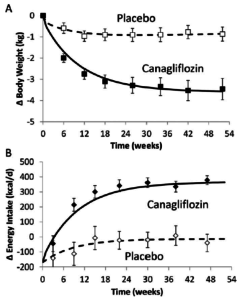
Figure 1: Weight loss (kg) compared to time (weeks) for placebo vs. Canagliflozin.
The fact that bodyweight ultimately stabilized at a new equilibrium point by the end of the study suggests that energy intake spontaneously increased to compensate for the calories lost in the urine. The researchers’ mathematical model showed that steady-state energy intake increased by approximately 350 kcal/d in the Canagliflozin group, whereas there was no significant change in energy intake in the placebo group by the end of the trial. This represented approximately 100 kcal increase in energy intake per kilogram of weight lost — an over threefold greater effect than the 30 kcal/kg/d decrease in energy expenditure that everyone seems to be so worried about.
This reflects a complex neurohormonal feedback system, integrated by the brain, that results in a proportional increase in appetite (and therefore energy intake) the more weight is lost. This helps to explain the common trajectory of real-world weight loss interventions, where initial progress is followed by plateau (when calorie intake has spontaneously increased to negate the initial calorie deficit) followed by gradual weight regain as appetite remains elevated.
The paper ends with a powerful quote:
“The few individuals who successfully maintain weight loss over the long term do so by heroic and vigilant efforts to maintain behavior changes in the face of increased appetite along with persistent suppression of energy expenditure (40) in an omnipresent obesogenic environment. Permanently subverting or countering this feedback control system poses a major challenge for the development of effective obesity therapies”.
So, what are the takeaways from this novel experiment? Most folks who go on a diet and lose weight will burn less calories as they become lighter, as discussed in our example of the person who lost 10kg now burning 300 calories less per day. When combined with a brain-mediated drive to increase calorie intake we can see how many dieters can fall short of their goal, which is backed up by evidence looking at the success of dietary interventions long term.
While this may seem pretty bleak, there is hope. The National Weight Loss Registry is comprised of data submitted from over 10,000 adults who have lost at least 30 pounds for a minimum of a year. When looking at this data we can see common behaviors that can help those who are dieting be successful such as:
- 98% of participants modified their food intake in some way to lose weight
- 94% increased their physical activity with 90% exercising an average of about 1 hour per day
- 78% eat breakfast every day.
- 75% weigh themselves at least once a week.
- 62% watch less than 10 hours of TV per week.
These behavioral changes can be very useful in practice and should be a part of a bottoms-up approach towards weight loss management. We encourage practitioners to consider these when working with clients and patients.
For more information, check out the paper below, our other articles on the topic, and our recent podcast. Thanks for reading!
References
- Polidori, David, et al. “How Strongly Does Appetite Counter Weight Loss? Quantification of the Feedback Control of Human Energy Intake.” Obesity, vol. 24, no. 11, 2016, pp. 2289–2295., doi:10.1002/oby.21653. Link.
